Prostate cancer is one of the most common cancers among men, affecting the prostate gland—a small, walnut-sized organ responsible for producing seminal fluid. The increasing prevalence of this disease has led to the evolution of various treatment options, with prostate cancer robotic surgery emerging as a groundbreaking and minimally invasive technique. This innovative approach has transformed how prostate cancer is treated, offering patients a range of benefits compared to traditional surgery. This blog explores prostate cancer robotic surgery, its advantages, and its impact on patient outcomes, including sexual function and urinary continence.
Understanding Prostate Cancer
Prostate cancer originates in the prostate gland, and its progression can vary significantly from slow-growing tumors to aggressive forms that spread quickly. Early detection is often the key to successful treatment. Clinically localized prostate cancer, where the cancer has not yet spread beyond the prostate gland, is the most common stage at diagnosis. For many men, treating prostate cancer at this stage with surgery or other therapies offers a high chance of recovery.
As technology in the medical field has advanced, so too have the methods used to treat prostate cancer. Robotic prostatectomy, a cutting-edge procedure, has gained prominence due to its precision, minimally invasive nature, and positive patient outcomes.
What Is Prostate Cancer Robotic Surgery?
Prostate cancer robotic surgery, also known as robotic radical prostatectomy, is a minimally invasive technique used to remove the prostate gland in patients diagnosed with prostate cancer. Unlike traditional open surgery, which requires a large incision, robotic surgery uses small incisions and is performed with the assistance of robotic arms controlled by the surgeon.
The robotic system enhances the surgeon’s ability to perform delicate and complex procedures, offering superior dexterity and control. During robotic prostate surgery, the surgeon operates from a console equipped with 3D imaging technology, allowing for greater precision and reduced risks of complications. This level of accuracy is particularly beneficial in preserving the nerves around the prostate gland, which are critical for maintaining erectile function and urinary continence.
The Evolution of Robotic Prostatectomy
 Robotic surgery has revolutionized the way prostate cancer surgery is performed. In the past, radical prostatectomy required a major surgery, which involved a long recovery period, significant blood loss, and higher chances of complications such as urinary incontinence and erectile dysfunction. The introduction of robotic-assisted surgery has mitigated many of these risks.
Robotic surgery has revolutionized the way prostate cancer surgery is performed. In the past, radical prostatectomy required a major surgery, which involved a long recovery period, significant blood loss, and higher chances of complications such as urinary incontinence and erectile dysfunction. The introduction of robotic-assisted surgery has mitigated many of these risks.
Robotic prostatectomy, also referred to as robotic-assisted prostatectomy or robotic radical prostatectomy, has quickly become the gold standard for treating prostate cancer. It allows for a more precise removal of the prostate gland while minimizing damage to surrounding tissues. The result is less blood loss during surgery, fewer complications, and a faster recovery for most patients.
Advantages of Prostate Cancer Robotic Surgery
- Minimally Invasive: One of the most significant advantages of prostate cancer robotic surgery is that it is minimally invasive. The use of small incisions reduces trauma to the body, which leads to less postoperative pain and faster recovery times. Unlike traditional prostate surgery, where a large incision is made in the lower abdomen, robotic prostate surgery requires only a few small keyhole incisions.
- Reduced Blood Loss: Blood loss during robotic-assisted prostate surgery is significantly lower compared to traditional open prostate cancer surgery. In conventional prostate removal surgery, the need for blood transfusion is higher, which can increase the risk of complications. Robotic surgery minimizes this need, reducing the chances of requiring a blood transfusion and lowering the overall risk associated with major surgery.
- Improved Precision: Robotic-assisted prostatectomy allows surgeons to operate with a high degree of precision. The enhanced visualization and dexterity provided by the robotic system enable the surgeon to avoid damaging critical structures around the prostate gland, such as the nerves responsible for sexual function and urinary continence. This increased precision results in better outcomes for patients, particularly in preserving erectile function and minimizing urinary incontinence.
- Faster Recovery: Most patients undergoing robotic-assisted prostate surgery experience a quicker recovery compared to those who undergo traditional surgery. The smaller incisions and reduced trauma to the body mean that patients can return to normal activities sooner. Additionally, the shorter hospital stay associated with robotic prostate surgery lowers the risk of postoperative infections and complications.
- Enhanced Visualization: The 3D imaging and magnification provided by the robotic system give surgeons a clear and detailed view of the surgical site. This level of visualization allows for meticulous dissection and removal of the prostate gland, reducing the risk of leaving behind any cancerous tissue. Enhanced visualization also aids in the safe and effective removal of lymph nodes during pelvic lymph node dissection, a procedure often performed alongside prostate cancer surgery.
The Procedure: How Robotic Prostatectomy Works
Robotic prostatectomy involves several key steps, all performed with the aid of the robotic system:
- Preparation: The patient is placed under general anesthesia, and several small incisions are made in the abdomen. These incisions are used to insert the robotic arms, which are equipped with surgical instruments.
- Robotic-Assisted Surgery: The surgeon sits at a console and controls the robotic arms with precise movements. The robot mimics the surgeon’s hand movements, allowing for fine control and precision. The surgeon views the prostate gland and surrounding tissues in real-time using a high-definition, 3D camera.
- Prostate Removal: The robotic arms are used to carefully dissect the prostate gland from surrounding tissues. In some cases, a pelvic lymph node dissection may be performed to check for the spread of cancer. The entire prostate gland is removed through one of the small incisions, and the surgeon takes great care to preserve the nerves responsible for sexual and urinary function.
- Post-Surgery: Once the prostate gland has been removed, the surgeon closes the incisions, and the patient is taken to the recovery room. A urinary catheter is usually placed to help the bladder heal, and this is typically removed after a few days.
Sexual Function and Urinary Continence After Robotic Prostatectomy
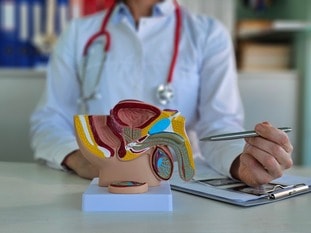 One of the primary concerns for men undergoing prostate cancer surgery is the impact on sexual function and urinary continence. These functions are closely related to the nerves and muscles around the prostate gland, which can be affected during surgery.
One of the primary concerns for men undergoing prostate cancer surgery is the impact on sexual function and urinary continence. These functions are closely related to the nerves and muscles around the prostate gland, which can be affected during surgery.
Robotic prostatectomy offers a significant advantage in this regard. The precision of the robotic system allows surgeons to spare the delicate nerves responsible for erectile function and urinary control. While some degree of erectile dysfunction and urinary incontinence may occur immediately after surgery, most patients experience improvement over time. In many cases, patients regain urinary continence within a few months, and sexual function can improve with the help of medications or therapies designed to aid erectile function.
Comparing Robotic Prostatectomy to Other Treatment Options
When considering prostate cancer treatment, patients often weigh the pros and cons of different surgical and non-surgical options. Traditional prostate surgery, laparoscopic radical prostatectomy, radiation therapy, and active surveillance are all valid treatments for localized prostate cancer. However, robotic prostate surgery offers unique benefits, especially for patients seeking a minimally invasive solution.
- Laparoscopic Radical Prostatectomy: Like robotic prostatectomy, laparoscopic surgery is minimally invasive and involves small incisions. However, laparoscopic surgery is typically performed without robotic assistance, which may limit the surgeon’s precision. Robotic-assisted surgery provides better visualization and dexterity, making it the preferred choice for many surgeons and patients.
- Radiation Therapy: Radiation therapy is another option for treating localized prostate cancer, especially for patients who may not be candidates for surgery. While radiation is less invasive than surgery, it can have long-term side effects, such as damage to surrounding tissues and organs. In contrast, robotic surgery allows for the precise removal of the prostate gland with minimal damage to surrounding tissues.
- Active Surveillance: For men with slow-growing or low-risk prostate cancer, active surveillance may be recommended. This involves closely monitoring the cancer without immediate treatment. While this approach avoids the risks of surgery, it may not be appropriate for patients with more aggressive forms of prostate cancer. For these patients, robotic-assisted surgery offers a curative option with fewer long-term side effects compared to traditional surgery.
Risks and Considerations
As with any major surgery, prostate cancer robotic surgery carries some risks. These include the possibility of infection, bleeding, and adverse reactions to anesthesia. Additionally, there may be a risk of blood loss, though this is significantly lower than with traditional surgery.
The most common postoperative issues include urinary incontinence and erectile dysfunction. However, as discussed earlier, robotic surgery helps mitigate these risks due to its precision in preserving the nerves around the prostate gland. Most patients see a gradual return to normal function over time.
It’s also important to note that not all patients are candidates for robotic prostatectomy. Factors such as the stage of cancer, the patient’s overall health, and the location of the tumor may influence the choice of treatment. Patients should thoroughly discuss with their healthcare provider to determine the best course of action.
Recovery and Long-Term Outcomes
Recovery after prostate cancer robotic surgery is typically faster and smoother compared to traditional open surgery. However, while the immediate recovery may be more comfortable, it’s important for patients to understand the various stages of recovery and the potential long-term outcomes associated with robotic prostatectomy. These include improvements in urinary continence, preservation of sexual function, and a quicker return to normal activities. Still, some patients may experience complications, which can vary depending on individual factors such as age, overall health, and the severity of the cancer. Understanding these recovery stages can help patients better prepare for life after prostate cancer surgery.
Immediate Postoperative Recovery
One of the key advantages of robotic-assisted prostatectomy is the use of minimally invasive techniques. Unlike traditional prostate surgery, which involves large incisions and longer recovery periods, robotic surgery requires only small keyhole incisions. This leads to less trauma to the surrounding tissues, which translates into less postoperative pain and a faster recovery.
Most patients who undergo robotic-assisted prostate surgery can expect to stay in the hospital for only one to two days, depending on their condition. Upon discharge, they are typically provided with a set of recovery instructions that cover wound care, activity restrictions, and managing any temporary side effects. A urinary catheter is usually placed during surgery to allow the bladder to heal, and it remains in place for about a week after the operation.
The initial recovery phase involves a gradual return to light activities. Patients are encouraged to walk and move around as soon as possible, as this helps reduce the risk of blood clots and improves circulation. However, heavy lifting and strenuous activities should be avoided for at least four to six weeks to prevent complications.
Management of Urinary Continence
One of the most common concerns following prostate cancer surgery is the impact on urinary function. The prostate gland is located near muscles and nerves that control the bladder, and surgery can sometimes disrupt these structures, leading to temporary or, in some cases, long-term urinary incontinence. However, thanks to the precision of robotic surgery, the risk of severe incontinence is significantly reduced compared to traditional surgery.
During a robotic radical prostatectomy, the surgeon can use the enhanced visualization provided by the robotic system to carefully preserve the structures involved in urinary control. This leads to a higher likelihood of maintaining urinary continence after surgery. Most patients experience some degree of urinary leakage in the weeks following the procedure, but this typically improves with time.
Many patients regain full control of their bladder within three to six months post-surgery. In cases where incontinence persists, pelvic floor exercises, such as Kegel exercises, may be recommended to strengthen the muscles responsible for bladder control. For most patients, these exercises are highly effective in restoring urinary continence, although it’s important to follow a consistent routine and consult with a healthcare provider or physical therapist for guidance.
Sexual Function and Erectile Dysfunction
Another major concern for men undergoing prostate cancer surgery is the potential impact on sexual function. The nerves responsible for erections are located near the prostate, and these nerves can be damaged during surgery, leading to erectile dysfunction. However, with robotic prostate surgery, surgeons have the precision needed to spare these nerves during the procedure. This nerve-sparing technique is particularly beneficial for preserving erectile function.
Despite the precision of the surgery, some patients may experience erectile dysfunction immediately after the procedure. This is often a temporary issue, as the body takes time to heal. Recovery of erectile function varies from patient to patient and depends on factors such as age, the extent of cancer, and the patient’s pre-surgery sexual function.
In many cases, erectile function begins to improve within six months to a year after surgery. Medications such as phosphodiesterase inhibitors (e.g., Viagra or Cialis) are often prescribed to aid in the recovery of sexual function. Additionally, other treatments such as vacuum erection devices or penile injections may be recommended for patients who require additional assistance in achieving erections.
It’s important to note that younger patients and those with good preoperative sexual function tend to recover erectile function more quickly than older patients or those with preexisting erectile issues. In some cases, full recovery may take up to two years, but many men can still experience satisfying sexual relationships post-surgery with the help of appropriate interventions.
Long-Term Outcomes and Cancer Control
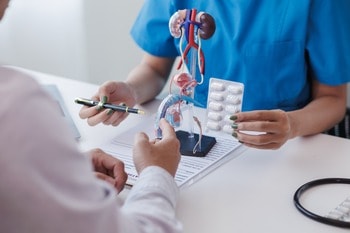 The primary goal of prostate cancer robotic surgery is to remove the cancerous tissue while minimizing the impact on the patient’s quality of life. The precision offered by robotic-assisted surgery allows for the complete removal of the prostate gland with a lower risk of leaving behind cancerous cells. This leads to excellent long-term cancer control, with many patients achieving cancer-free survival following the procedure.
The primary goal of prostate cancer robotic surgery is to remove the cancerous tissue while minimizing the impact on the patient’s quality of life. The precision offered by robotic-assisted surgery allows for the complete removal of the prostate gland with a lower risk of leaving behind cancerous cells. This leads to excellent long-term cancer control, with many patients achieving cancer-free survival following the procedure.
For patients with clinically localized prostate cancer, the long-term outcomes are especially favorable. Studies have shown that robotic radical prostatectomy is highly effective in treating localized prostate cancer, with survival rates comparable to or better than those of traditional surgery. The procedure also significantly reduces the likelihood of cancer recurrence, especially when performed by an experienced surgeon.
In some cases, a pelvic lymph node dissection may be performed during the surgery to check for any spread of cancer beyond the prostate. If cancer cells are found in the lymph nodes, additional treatments such as radiation or hormone therapy may be recommended to ensure long-term cancer control.
Impact of Benign Prostatic Hyperplasia on Recovery
For patients who had preexisting conditions such as benign prostatic hyperplasia (BPH) before surgery, recovery may present additional considerations. BPH is a non-cancerous enlargement of the prostate that can cause urinary symptoms, such as difficulty urinating or frequent urination. If the patient had BPH before surgery, the removal of the prostate during a robotic prostatectomy can provide relief from these symptoms, leading to improved urinary function in the long term.
However, BPH can complicate the surgery itself, as an enlarged prostate can make the procedure more challenging. The precision offered by robotic surgery is particularly beneficial in these cases, as it allows for careful dissection of the enlarged prostate tissue without causing damage to surrounding structures. Patients with BPH can still expect a favorable recovery, though it’s essential to follow their surgeon’s recommendations closely and attend follow-up appointments to monitor their progress.
Conclusion: The Future of Prostate Cancer Treatment
Prostate cancer robotic surgery represents a significant leap forward in the treatment of prostate cancer. The minimally invasive nature of the procedure, combined with the precision and control offered by robotic systems, makes it an attractive option for many patients.
Overall, the combination of robotic-assisted surgery, advances in other treatment areas, and personalized medicine represents a new era in the fight against prostate cancer. For men diagnosed with this condition, the future holds great promise, offering them more effective treatments, fewer side effects, and a better chance at living cancer-free. The continuous evolution of prostate cancer therapies, including the further refinement of robotic prostatectomy, ensures that patients will have access to the best possible care, setting a new standard for cancer treatment in the 21st century.
References
https://journals.lww.com/co-urology/FullText/2018/03000/Robotic_surgery_in_urology__facts_and_reality_.10.aspx
https://bjui-journals.onlinelibrary.wiley.com/doi/abs/10.1111/bju.12850
https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/robotic-prostatectomy


