Can a distended bladder return to normal? If you are asking this question, you’re not alone. Many face this troubling condition, wondering if their bladder can regain its usual function. In this discussion, we delve into the causes of bladder distention, evaluate various treatment options, and explore how these interventions can help the bladder recover. Join us as we uncover insights into the potential for a distended bladder to return to normal, guided by medical expertise and patient experiences.
Can a Distended Bladder Return to Normal?
Yes, a distended bladder can often return to normal, depending on the underlying cause of the enlargement and the effectiveness of the treatment approach. The ability of the bladder to recover normal function is influenced by several factors, including the duration and severity of the enlargement, the general health of the patient, and how quickly treatment is initiated.
Bladder Distention Causes
Bladder distention, characterized by an abnormal enlargement of the urinary bladder, arises from various medical issues that disrupt normal urination. Understanding these causes is essential for effective diagnosis and management of bladder distension.
Obstructive Causes
One of the primary reasons for bladder distention is an enlarged prostate in men, which can press against the urethra and obstruct urine flow. Similarly, physical blockages in the bladder lining the urinary tract, such as kidney stones, tumors, or strictures, can also impede urine flow, causing the bladder to retain more urine than normal and become distended.
Neurological Causes
Conditions that affect the nervous system can significantly impact bladder function. For instance, multiple sclerosis or spinal cord injuries can interfere with the nerve signals that are crucial for bladder control, leading to neurogenic bladder. This dysfunction prevents the bladder from emptying, causing urine retention and subsequent enlargement.
Functional Causes
The weakening of the bladder muscles or dysfunction in the pelvic floor muscles can compromise the bladder’s ability to empty properly. Age-related changes, injury, or conditions like diabetes can lead to weakened bladder muscles, while childbirth, surgery, or pelvic trauma can affect the pelvic floor muscles. Both scenarios contribute to inefficient bladder emptying.
Infection and Inflammation
Infections such as urinary tract infections can cause swelling and irritation of the bladder walls. This inflammation can temporarily reduce the bladder’s capacity to contract properly, leading to incomplete emptying and increased urine volume that contributes to bladder distention.
The Impact of Bladder Distention

Bladder distention can significantly impact an individual’s health and quality of life. Understanding its effects is crucial for effective management, proper treatment, and minimizing long-term complications.
Urinary Symptoms: Bladder distention often leads to uncomfortable and sometimes painful urinary symptoms. Individuals may experience frequent urination, a constant feeling of a full bladder, and difficulty initiating urination. Severe bladder distention can result in acute urinary retention, where the patient is unable to urinate at all, requiring immediate medical attention.
Increased Risk of Infections: A distended bladder can lead to stagnant urine within the body. This stagnation can cause the urinary system to become a breeding ground for bacteria, increasing the risk of urinary tract infections (UTIs). Recurrent infections can further damage the bladder and urinary tract, compounding the distress and potential for chronic health issues.
Effect on Kidney Health: Prolonged bladder distention can exert pressure back towards the kidneys. This pressure can interfere with kidney function and potentially lead to hydronephrosis (kidney swelling), where urine fails to drain properly from the kidney due to chronic bladder distension. Over time, this can cause kidney damage and, in severe cases, renal failure.
Impact on Quality of Life: The symptoms of bladder distention can significantly impair an individual’s quality of life. The discomfort and frequent need to urinate can disrupt sleep, complicate social engagements, and diminish overall mental well-being. Chronic pelvic pain and social embarrassment are common, and the condition can negatively affect personal life including relationships and employment.
Long-Term Health Complications: If left untreated, bladder distention can cause more severe health issues, including bladder damage and chronic urinary retention. These complications may require more invasive treatments such as catheterization, surgery, or other medical interventions to manage the symptoms and prevent deterioration of health.
Assessing the Severity of Bladder Distention
Assessing the severity of bladder distention is crucial for forming the appropriate treatment plan and preventing further complications. This evaluation typically involves a combination of clinical assessment, patient symptoms, and diagnostic tests:
Clinical Symptoms: The initial assessment focuses on the patient’s symptoms. Key indicators include the frequency and urgency of urination, the presence of pain or discomfort in the pelvic area, and the inability to empty the bladder. Unusual symptoms such as painful urination or severe discomfort may indicate a more severe distention.
Physical Examination: A urologist may conduct a physical examination to evaluate tenderness or swelling in the abdominal and pelvic areas, which can suggest an overly distended bladder. Palpation and percussion of the bladder can help determine its size and level of fullness.
Medical History: Understanding the patient’s history is essential. Factors such as previous episodes of urinary retention, underlying medical conditions (e.g., diabetes, neurological disorders), and current medications are considered to assess risk factors and potential causes of bladder distention.
Diagnostic Tests
- Ultrasound: This imaging test is commonly used to visualize the bladder and assess the amount of residual urine after urination, helping to quantify the degree of distension.
- Urodynamic Tests: These tests measure the bladder’s ability to empty steadily and completely, providing data on bladder strength and urinary flow.
- Cystoscopy: In some cases, a cystoscope may examine the interior of the bladder and urethra. This is particularly useful if there is a suspicion of structural abnormalities or blockages.
Severity Classification: Based on these assessments, other symptoms of bladder distention can be classified from mild to severe. Mild cases may only require lifestyle changes and minimal intervention. In contrast, severe cases might necessitate more aggressive treatments such as catheterization or surgery to relieve the obstruction and prevent damage to the bladder and kidneys.
Treatment Options for Restoring Bladder Function

Restoring bladder function when facing issues like distention involves a variety of treatment plans tailored to manage the underlying cause and severity of the condition. Here’s a comprehensive overview of the treatments available:
Behavioral Interventions
For mild cases, simple lifestyle changes can significantly help. This includes timed urination schedules to train the bladder to empty regularly, performing pelvic floor exercises to strengthen the muscles and support better bladder control, and managing fluid intake to optimize bladder function.
Medications
Certain drugs can help manage symptoms of bladder distention. Anticholinergic medications can reduce bladder spasms and urgency, while alpha-blockers can improve urine flow in men with prostate issues that affect bladder emptying. Medications that alter nerve impulses to the bladder for the neurogenic bladder can be effective.
Catheterization
Intermittent or continuous catheterization may be necessary for patients who cannot empty their bladder. This method directly removes urine from the bladder, preventing overdistention and reducing the risk of infections and other complications.
Surgical Interventions
Surgery might be required in severe cases or when physical obstructions or significant structural problems cause the enlargement. Procedures may include:
- Bladder Augmentation: Surgically increasing the bladder’s capacity.
- Prostate Surgery: For men, reducing prostate size if it’s impeding urine flow.
- Urethral Stricture Surgery: Removing or dilating urethral strictures that block urine flow.
Electrical Stimulation
For some types of neurological conditions of bladder dysfunction, particularly due to nerve damage, electrical stimulation of the nerves controlling the bladder can improve function. This is often used for conditions like spinal cord injuries or severe diabetes.
Biofeedback
This therapy uses monitoring devices that help patients become aware of their body’s body toning, enabling them to improve control of their pelvic floor muscles.
Management of Associated Conditions
Addressing and treating any underlying conditions contributing to bladder dysfunction, such as diabetes, neurological disorders, or urinary infections, is crucial for restoring normal bladder function.
Lifestyle Adjustments and Home Remedies to Support Recovery

Adopting certain lifestyle adjustments and utilizing home remedies can significantly support recovery and enhance the management of bladder-related issues. Here are practical strategies that can be easily integrated into daily routines:
Hydration Management: Proper hydration is crucial. Drinking enough water helps remove bacteria from the urinary tract by flushing it out. This helps avoid developing infections that can exacerbate bladder problems. However, balancing fluid intake is important to avoid overwhelming a sensitive bladder.
Dietary Considerations: Certain foods and beverages can irritate the bladder and should be avoided. These include caffeine, alcohol, spicy foods, and acidic fruits. Instead, focus on a bladder-friendly diet that includes high-fiber foods, which prevent constipation—a condition that can put extra pressure on the bladder.
Timed Voiding: Establishing a routine for urination can help manage bladder distention. Timed voiding involves urinating at regular intervals and can be modified based on individual needs to prevent the patient’s bladder from becoming too full.
Pelvic Floor Exercises: Exercises like Kegels, which strengthen pelvic floor muscles, can significantly enhance bladder control. This improvement supports the bladder’s ability to return to normal function. These exercises are especially useful for individuals experiencing stress urinary incontinence or a weak pelvic floor.
Stress Reduction: Stress can exacerbate many health issues related to bladder function. Techniques such as yoga, meditation, and deep-breathing exercises can help control stress levels and positively impact overall urinary health.
Avoid Bladder Irritants: Smoking is a major irritant that can worsen bladder conditions and hinder recovery. Quitting smoking is highly recommended to improve bladder health and avoid the risk of further complications.
Temperature Therapy: Applying a warm compress to the pelvic area can help relieve symptoms of pain and discomfort associated with bladder issues. This can be particularly soothing during episodes of bladder spasms or after performing pelvic exercises.
Regular Exercise: Regular physical activity contributes to keeping the body healthy and reduces the risk of bladder problems by improving overall muscle tone and bladder control.
Monitoring and Managing Long-Term Bladder Health
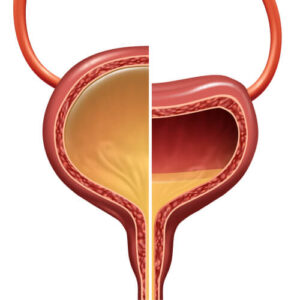
Monitoring and managing long-term bladder health is crucial for preventing recurring issues and maintaining overall wellness, especially for the extended bladder. Here are effective strategies for ensuring sustained bladder function and health:
Regular Medical Check-ups: Visiting the urologist consistently is essential for monitoring bladder health, especially if you have a history of bladder issues. These check-ups typically involve a physical examination and urine tests to identify infections or other abnormalities. Additionally, ultrasound imaging may be used to visualize the bladder’s structure and function.
Maintain a Bladder Diary: Keeping a diary can help track patterns in urination, such as frequency, urgency, pain, and any incontinence episodes. This record is invaluable for doctors to understand how treatments are working or if adjustments are needed.
Hydration and Diet: Consistently managing fluid intake to ensure proper hydration without overloading the bladder is key. Additionally, a diet low in irritants like caffeine, alcohol, spicy foods, and acidic foods can help maintain bladder integrity and reduce irritation.
Pelvic Floor Muscle Training: Regular pelvic floor exercises strengthen the muscles that support bladder control, crucial for preventing incontinence and supporting bladder function. These exercises are especially important for individuals who have experienced childbirth or surgery or who are aging.
Manage Constipation: Chronic constipation can pressure the bladder and exacerbate urinary problems. Managing this through a high-fiber diet, adequate hydration, and regular exercise is important for bladder health.
In conclusion, addressing whether a distended bladder can return to normal is essential for those experiencing this condition. With the right treatment and healthy lifestyle, many individuals see significant improvements in bladder function. Recovery is a tangible goal that can be achieved by understanding the underlying causes and engaging in proactive health management. Suppose you or someone you know is dealing with bladder distention. In that case, consulting with healthcare professionals is critical to creating a tailored approach that encourages a return to normal bladder health.
References
Distended Bladder: Causes, Symptoms & Treatment
https://my.clevelandclinic.org/health/diseases/distended-bladder
Enlarged Bladder: Symptoms, Treatments, and Causes
https://www.healthline.com/health/enlarged-bladder
Treatment Options May Be Available for Patient with Poor Bladder Function
https://newsnetwork.mayoclinic.org/discussion/treatment-options-may-be-available-for-patient-with-poor-bladder-function/
The bladder can regenerate like nobody’s business, and now we know why
https://news.wisc.edu/the-bladder-can-regenerate-like-nobodys-business-and-now-we-know-why/
Distended bladder presenting with constipation
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3398309/


